Federated Health Charities’ mission is to improve the health and quality of life of all Ontarians by supporting 21 different health charities providing critical services to those experiencing, or affected by, illness. We believe education and prevention are key parts of supporting the health of our communities so our weekly Health Hint series strives to provide tangible and easy to implement hints and tips on how to maintain your health, prevent disease, and enjoy increased quality of life. Check out our latest Health Hint on external otitis. We hope you find it helpful. If you would like to join our efforts to support the health of Ontario please consider a donation to Federated Health Charities.
The ear is made up of three distinctive parts: the external ear, the middle ear, and the inner ear. The external part of the ear is the part of the ear one can see and is called the pinna (auricle). The external ear is extended to the ear canal (external auditory canal) and the ear drum (called outer surface of tympanic membrane). There are multiple ear disorders, but we are going to focus on external otitis.
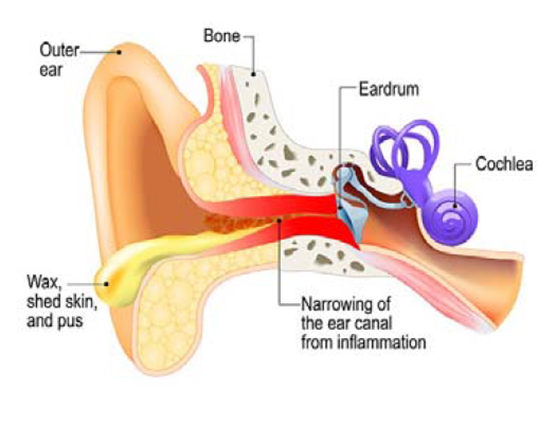
Cause of External Otitis
External Otitis (EO) is inflammation (swelling) of the external auditory canal secondary to fungal or bacterial infection. EO, also known as swimmer’s ear, is believed to be most commonly the consequence of local trauma to the external auditory canal. For example, fingers, sharp objects, or cotton tipped applicators inserted too deep in the ear can cause the trauma. In some cases, prolonged exposure to moisture (e.g. underwater swimming, humid environment, and diving) promotes soaking of the thin skin lining the ear canal, permitting bacteria to enter and grow as the bacteria and fungi grow in warm, dark, and easily moist environment. External otitis usually occurs in summer season because adults and children are swimming. The major microscopic organisms isolated from patients with swimmer’s ear are Pseudomonas aeruginosa (20-60%)and Staphylococcus aureus (10-70%).
EO can be classified as acute diffuse, acute localized, chronic, eczematous, or necrotizing. Acute EO is an infective condition due to bacteria or fungi and the chronic form of EO may be in the form of contact dermatitis or atopic dermatitis. In some cases, both forms of the conditions may be existed together.
- Acute diffuse: The predisposing factor of this group of EO is too little earwax (cerumen), excessive earwax, chronic skin disorders, trauma to the EAC, hairy canal and hearing aids narrowing.
- Acute Localized EO (Furunculosis): A bacterium called S. aureus is responsible for this condition and mainly infects the ear canal hair follicles. Localized pain, swelling, itching, redness, and possibly abscess may be experienced.
- Chronic EO: characterized as a stiffening of the EAC skin and swelling. There is usually continual severe itching (pruritus), slight discomfort and dry, blistered skin in the EAC with absence of earwax. Chronic EO is non-infective resulting from allergic dermatitis.
- Eczematous EO: May be due to a variety of skin disorders. The common symptom is severe itching, redness, swelling, discharge, and crusting. There is also the possibility of fungi and bacteria.
- Necrotizing (Malignant) EO: The infection may extend to the bone, especially in patients with diabetes and low immune system.
General Symptoms
Early symptoms of EO include itching and a sensation of fullness and pressure in the ear, followed by otic discharge (otorrhea), pain and a possible decrease in hearing. The pain in the ear (otalgia) may be intense especially when the jaw or outer ear is touched or moving. The patient needs to visit their doctor if symptoms extend to severe pain, deafness, blocked ear, dizziness, tinnitus, discharge, neck stiffness, bleeding, nausea and vomiting or injuries. Patient may also have symptoms in other parts of the body as well. External otitis may contain yellow, bluish green, or grey elements, and fungal EO usually produces white debris. The disease usually occurs in children ages 7-12 and occurrence declines after age 50.

Non medication measures
- Cleansing of the ear canal is necessary for creating a good condition for topical medication. Cleansing is performing by a healthcare practitioner with appropriate training or a specialist.
- Avoid the use of cotton swabs.
- After bathing or swimming the ear can be cleaned by using a blow dryer on the low power setting. During medication cycles (7-10 days) avoid water sports.
Treatment
External otitis with bacterial or fungal infections can be treated by antibiotics or corticoids prescriptions. Topical treatment (e.g. antibiotic or non-antibiotic eye/ear drops) is the first line of treatment, but some patients may require systemic treatment. Discontinuation of mechanical trauma such as swimming until resolution of the infection is required. Antibiotics are not given when infection is not responsive with primary treatment options or the infection affects middle ear. External otitis should not be self-treated.
One of the FDA approved products is an ear drying agent called isopropyl alcohol 95% in anhydrous glycerin 5% and is for use in patients 12 years of age or older. A home remedy is a solution of 50/50 isopropyl alcohol and white vinegar that may be used for drying of the ear. All at-home treatment options should first be discussed with your healthcare practitioner.
The best option is the prevention of the problem all together. Behaviors that can cause mechanical trauma, such as using cotton tipped applicators or fingers in your ear, should be stop immediately. After bathing or swimming, water should be expelled from the ears by using a clean towel around the edges of the ears or by using a blow dryer.
We hope you liked out latest Health Hint!
Written by Mohammad Zafar Omari MSc, MBA, PMP
References
CTMA 2019 ‑ Compendium of Therapeutics for minor ailments. Ear Conditions.
Comprehensive Pharmacy Review for Naplex, eight editions. Chapter 19
Managing Symptoms in the Pharmacy, Alan Nathan. Chapter 5